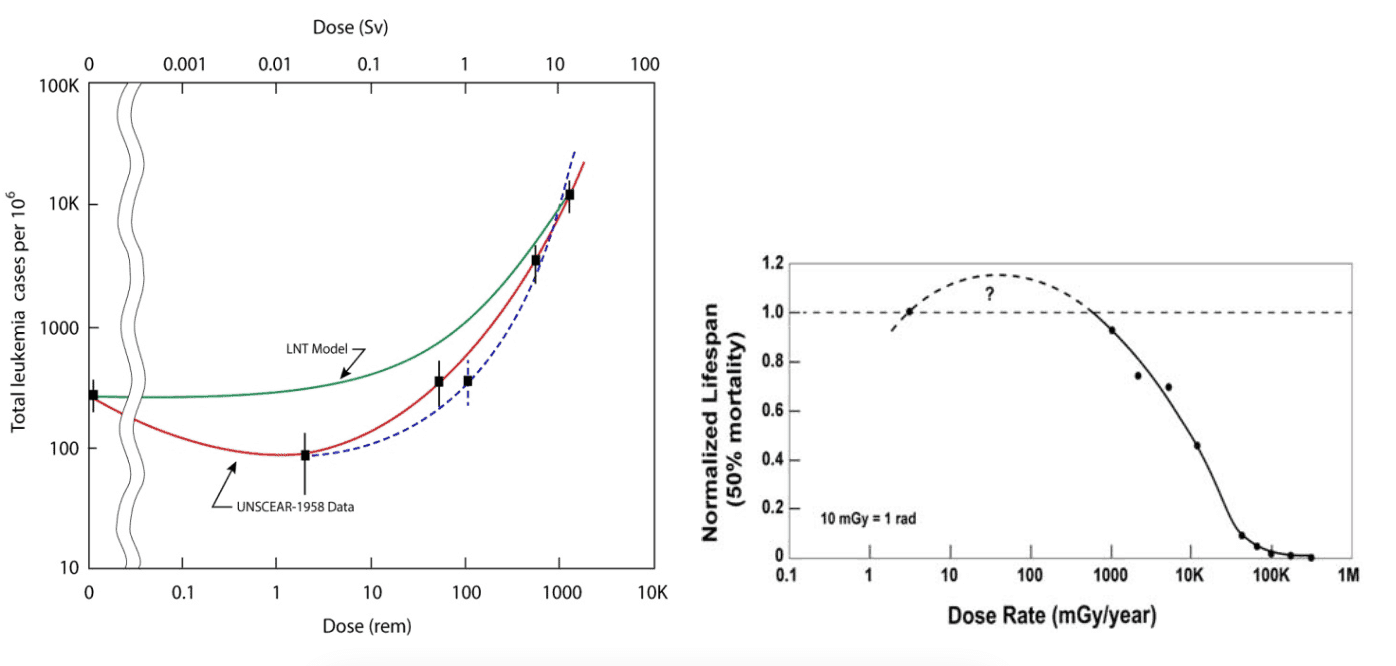
Displacing LNT assertion with evidence
A joint ANS/HPS (American Nuclear Society/Health Physics Society) meeting titled “Applicability of Radiation Protection Models to Low Dose Protection Standards” (hashtag #LowDose2018) will kick-off tonight. This much anticipated event has attracted 200 medical, radiation and nuclear energy experts to the booming metropolis of Pasco, WA. The site is appropriate, Pasco is one of the three…