Using X-rays To Treat Inner Ear Infections and Deafness
Dr. Edward Calabrese and G Dhawan have published an article titled Historical use of x-rays: Treatment of inner ear infections and prevention of deafness in Vol 33(5) of Human and Experimental Toxicology, May 2014.
Abstract
Purpose: This article provides an historical assessment of the role of radiotherapy in the treatment of inner ear infections.Materials and methods: The research utilized a literature-based evaluation of the use of x-rays during the first half of the 20th century on the treatment of otitis media (OM), mastoiditis, and cervical adenitis and their impact on the occurrence of deafness.
Results: X-Rays were consistently found to be effective as a treatment modality at relatively low doses, in the range of 10–20% of the skin erythema dose, rapidly reducing inflammation, and accelerating the healing process. The mechanistic basis of the clinical successes, while addressed by contemporary researchers, is evaluated in the present article in light of current molecular biology advances, which indicate that clinically effective low doses of ionizing radiation act via the creation of an anti-inflammatory phenotype in highly inflamed tissue.
Conclusions: X-Ray treatment of OM, mastoiditis, and cervical adenitis was widely accepted in the first half of the 20th century by clinicians as an effective treatment when administered within an appropriate dosage range.
The paper summarizes results from a number of medical papers published mostly during the period from 1920-1940, though there are some from as early as 1902 and as late as the mid 1960s.
In a related effort seeking effective treatments for lymphoid tissue-related hearing loss, Samuel J. Crowe at the Johns Hopkins University developed treatments using radium implants that showed impressive results.
Based on extensive clinical experience, they concluded that the most efficient treatment of hearing impairment due to excessive lymphoid tissue is irradiation with radium or x-rays. So striking were the findings of this clinical research that they claimed there was the potential to reduce the number of deaf adults in the next generation by 50%.
The success led to numerous discussions about the best treatment regimes, the most effective doses, and the relationship of patient ages to doses and results. Not surprisingly, critics also asked questions about the side effects of ionizing radiation.
There also emerged concern over whether there might be possible long-term effects related to the exposure to the ionizing radiation. This was especially the case for physicians and their assistants who were handling the radium on a daily basis while treating many patients. Further concerns were raised with respect to the long-term effects on patients, with particular concern for brain and thyroid. Table 3 summarizes the long-term studies conducted on patients irradiated with nasopharyngeal radium to treat ear dysfunctions. Such studies did not detect a definitive link between nasopharyngeal irradiation and any disease, including cancer, suggesting the capacity to estimate an upper bound risk for such procedures.
Here is an image version of the referenced Table 3 from the paper.
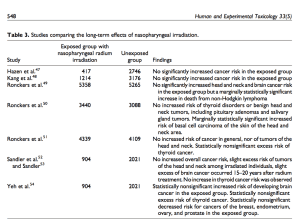
The paper authors note that treatments using therapeutic x-rays lost favor with the development of improved antibiotics and surgical procedure advances. When the treatments lost favor, there was no proposed theory to explain why they seemed to work so well; at that time, doctors were often satisfied to find effective treatments without needing to have a detailed understanding of exactly why they worked.
Recent findings have emerged, which may offer insight into this matter. In general, low doses of x-rays have been shown to affect the development of a highly integrated anti-inflammatory phenotype…This anti-inflammatory phenotype is a con- sistent feature when low doses of ionizing radiation are administered to tissues with substantial inflammation. Mechanistic studies with multiple animal and cell models have confirmed the consistency of these observations accounting for the protective effects of low-dose ionizing radiation in animal models with various types of inflammatory disease such as arthritis.
Calabrese and Dhawan did not specifically point out that the increasing fear of radiation and the imposition of the linear no threshold (LNT) dose response assumption in radiation protection regulations may have also played a role in discouraging doctors from administering radiation to cure infections and inflammation.
However, they did note that it might be time to reconsider using ionizing radiation treatments in an era with an increasing number of “antibiotic-resistant disease-causing microbial strains.”
Please use the contact form if you would like additional information about the paper.

Rod,
I searched in the Journal of Historical Toxicology, and the same authors have also published papers about x-ray treatment of sinus infections, and pneumonia as well. It looks like there is merit for further investigation to see if there are better outcomes compared to antibiotics, and if the risks outweigh the probability of future cancer rates. (probably the benefits outweigh the risks).
I appreciate you writing this article and bringing it more out in the open.
Best Regards
Jay Bryner
That’s exactly it, Jay. Unfortunately some will reject such study because for them it’s just LNT denial, but it’s perfectly possible for the treatment to have both a positive immediate impact, and a negative LNT long term impact, *with the immediate benefits outweighing the risks*.
The situation is very similar to the experiments of Dr. Kiyohiko Sakamoto for half body radiation, with the difference that in the case of Sakamoto, it should be obvious how much lowering the risk of metastasis outweighs the risks of longer term LNT induced cancer :
https://atomicinsights.com/dr-kiyohiko-sakamoto-low-dose-radiation-used-as-cancer-treatment/
After some research I found that some others have made similar experiment, but many have quickly stopped them despite encouraging early results ( see for example http://www.ncbi.nlm.nih.gov/pubmed/19478704 “Half-body irradiation: a safe and acceptable treatment” and http://www.ncbi.nlm.nih.gov/pubmed/18979285 “Half body irradiation of patients with multiple bone metastases” ).
However it’s not a good thing either to simply ignore that several studies have indeed linked such therapeutic radiation exposure with later increased cancer rate.
Here from Melvin Griem : http://jnci.oxfordjournals.org/content/86/11/842.abstract “Cancer Following Radiotherapy for Peptic Ulcer”
And here from Ron E : http://www.ncbi.nlm.nih.gov/pubmed/2594972 “Thyroid neoplasia following low-dose radiation in childhood”
@jmdesp
I think I am finally beginning to understand that I have a completely different view of the words “significant” and “greatly” than epidemiologists – who are essentially statisticians.
Here is an example statement from the abstract of the Griem paper:
Read that again. Radiation induced stomach cancer was 1/4 of 1 death per 10,000 persons per year per Gy, yet the author calls that “greatly” enhanced. By the way, the study methodology used was to dig through medical records of people who were already dead.
I thinking they were mostly all people with pre existing serious medical conditions as well. Especially a history of cancer. It was a very odd choice of specific words, by people that know better, for a situation that did not fit.
The numbers raise two questions.
1… How many Gy for average treatment?
2… Does alternate treatment have greater or lesser risk?
Those certainly are relevant questions.
Rod,
A heads-up on this topic.
Page C3 of the April 12-13 Wall Street Journal has a piece by Craig Nelson entitled “A Radiation Reality Check”
You have probably seen it, but there was nothing today in your Twitter feed about it.
Rick
So, considering antibiotic-resistant bacteria, nuclear technologies and therapeutic radiotherapy/selective use of ionizing radiation might hold “world-saving” potential in terms beyond simply sufficient power supplies?
And demonization of these technologies is considered “en vogue” by a non-insignificant proportion of our population?
Something is grossly amiss in terms of weighing risk assessments in this day and age.
It hit me a few days ago that far far more people have been helped by Radiation than harmed, even when including instances of its worse misuse. Several orders of magnitude more. Thinking of it in terms of a “necessary evil” just with respect to energy is inappropriate and wrong. It is part of what makes our reality; and a wonderful set of tools and resources.
I think we will see a needed reboot soon when it comes to opinion and the value and importance of radiation. At least I hope it happens and look forward to the coming Version 2.0 of the Atomic Age.
Rod,
Do you know of any ongoing studies that are further trialing this method for deaf patients? What about congenital deafness – is there relevance for those patients? Or is it only used in conjunction with preventing deafness?
Thanks,
Rachael
WVSOM, OMS-I
Class of 2018